How to Use Clinical Data to Do Retrospective Cohort Study?
-
摘要: 临床病例资源丰富, 但往往存在基线资料不全、非随机分组导致混杂因素多、失访率高等问题, 限制了临床医生利用这些数据开展研究。采用限制、配对、分层、多因素分析、倾向性评分等多种方法可以克服已有临床病例资料的固有缺陷, 从而得出可靠结论。本文从队列研究的设计、分析、论文撰写等方面阐述如何进行高质量的临床研究。Abstract: Clinical data are abundant, but there are some problems that limit clinicians' use of these data for clinical research, such as incomplete baseline data, confounding bias due to nonrandom grouping, and higher loss of follow-up. The inherent defects of retrospective design can be overcome by limitations, matching, stratification, multivariate analysis, propensity score, and other methods. This article elaborated how to do a high-quality cohort study from the perspectives of design, analysis and paper writing.利益冲突 无
-
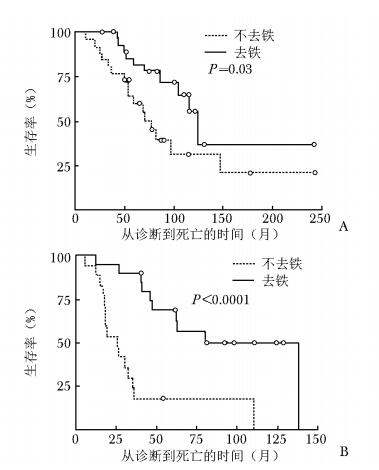
图 1 去铁治疗和不去铁治疗对骨髓增生异常综合征患者生存期的影响[4]
A.红细胞输注量≤3 U/月; B.红细胞输注量>3 U/月
表 1 HLA不相合活体肾移植患者与配对对照组的临床特征比较[3]
配对因素 HLA不相合活体肾移植
患者(n=1025)单纯等待未进行肾移植的
对照组1(n=5125)等待后进行HLA相合死亡供体
肾移植的对照组2(n=5125)移植时年龄(x±s, 岁) 45.0±12.8 45.9±12.1 46.6±12.0 女性患者[n(%)] 687(67.0) 3444(67.2) 3452(67.4) 黑人患者[n(%)] 168(16.4) 844(16.5) 840(16.4) 既往进行过肾移植的次数[n(%)] 0 612(59.7) 3323(64.8) 3321(64.8) 1 350(34.1) 1584(30.9) 1552(30.4) 2 57(5.6) 202(3.9) 231(4.5) ≥3 6(0.6) 16(0.3) 21(0.4) 中位抗体水平[M(Q), %] 66(22, 94) 68(20, 95) 68(21, 95) 糖尿病[n(%)] 210(20.5) 1047(20.4) 1047(20.4) 肾脏替代治疗时间(x±s, 年) 7.3±7.6 7.3±7.4 7.4±7.4 HLA:人类白细胞抗原 -
[1] Schulz KF, Grimes DA.《柳叶刀》临床研究基本概念[M].王吉耀(译).北京:人民卫生出版社, 2010:4-9. [2] 曾于珍, 陈世耀.临床研究结局指标选择与样本量估计[J].协和医学杂志, 2018, 9:87-92 [3] Orandi BJ, Luo X, Massie AB, et al.Survival Benefit with Kidney Transplants from HLA-Incompatible Live Donors[J].N Engl J Med, 2016, 374:940-950. [4] Rose C, Brechignac S, Vassilief D, et al.Does iron chelation therapy improve survival in regularly transfused lower risk MDS patients? A multicenter study by the GFM (Groupe Francophone des Myélodysplasies)[J].Leuk Res, 2010, 34:864-870. [5] Gowanlock Z, Sriram S, Martin A, et al.Erythropoiesis-stimulating agents in elderly patients with anemia:response and cardiovascular outcomes[J].Blood Adv, 2017, 1:1538-1545. [6] Sasaki K, Jabbour EJ, Ravandi F, et al.Hyper-CVAD plus ponatinib versus hyper-CVAD plus dasatinib as frontline therapy for patients with Philadelphia chromosome-positive acute lymphoblastic leukemia:A propensity score analysis[J].Cancer, 2016, 122:3650-3656. -


 作者投稿
作者投稿 专家审稿
专家审稿 编辑办公
编辑办公 邮件订阅
邮件订阅 RSS
RSS


 下载:
下载: